The number of GPs in the UK is falling in a sustained way for the first time in more than 50 years, according to new research.
Analysis by the Nuffield Trust on behalf of the BBC shows that there are now 60 GPs per 100,000 people in the UK – which is down from 64 just five years ago and means that the average doctor now has 125 more patients to look after than they did in 2014.
If the overall total of GPs had actually kept pace with population growth since 2014 then there would have needed to have been 3,400 more people in the profession.
This relative-to-population fall comes despite a rise of about half a million GP appointments in November 2018 compared to the previous November.
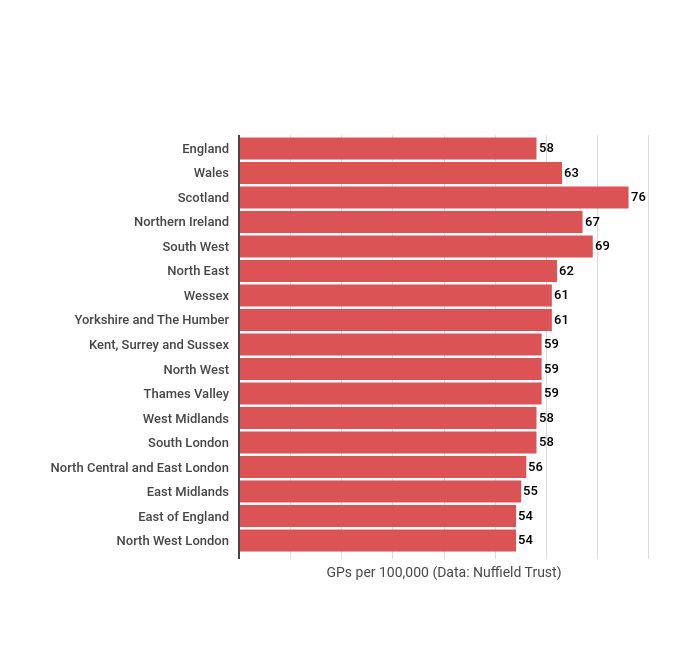
Regional figures also show a big disparity in different parts of the UK, with the East of England and North West London having just 54 GPs per 100,000 people compared to 76 in Scotland.
‘We need to keep skilled GPs in the profession’
MDS CEO Rohan Simon said: “This analysis shows it’s vitally important that we look after our existing GPs and keep skilled people in the profession. Medical Defense Society was established to stand up for GPs and help to ease the burden of indemnity costs, one of the factors that was contributing to GPs leaving their roles.
“This continues to be our mission as we offer the continued support and advice that GPs need for all of the important work they do that falls outside of the state backed indemnity scheme.
“We hope that more can be done to look after GPs and ensure that this fall reverses.”
Nuffield Trust director of strategy Helen Buckingham said that within the next five years the UK could be 7,000 GPs short. She pointed to a number of factors causing the drop in numbers including:
- the after-effect of a decrease in training places
- the number of GPs who have taken early retirement
- the trend of people leaving after they’ve qualified without going on to work as an NHS GP
The BBC noted that the NHS had previously been struggling to attract junior doctors to become GPs, with as many as one in ten training places empty.
That issue has eased now, and the 3,500 trainee posts taken up last year is up 800 on 2014. However, with it taking three years to train a junior doctor to become a GP, that will take a while to filter through.
‘Disheartening but not surprising’
Professor Helen Stokes-Lampard, Chair of the Royal College of GPs, said: “These figures are disheartening but will be unsurprising for GPs – and their patients – across the country who are feeling the impact of relentless workforce pressures in general practice on a daily basis.
“There is some excellent work ongoing to boost recruitment into general practice and as a result we have more GPs in training that ever before. But GPs cannot be trained overnight, and whilst we wait for the next generation of family doctors to enter the workforce, existing GPs and our teams are struggling to manage escalating workloads without enough time or the resources to deal with them.
“Demand for GP services is escalating both in terms of volume and complexity – and when this is compounded by falling GP numbers, it creates a perfect storm that is leading to GPs becoming stressed and burning out, and in many cases leaving NHS general practice far earlier than they might otherwise have done.
“More must be done to keep our hard-working, experienced GPs in the profession for longer – not only are they vital to delivering vital care to over a million patients a day, but they have a huge amount of wisdom to impart to new colleagues.”
Measures needed to help GPs
GP numbers were falling in the late 1960s but then grew continuously for about four decades before peaking at 66.5 in 2009. Numbers have now fallen for four consecutive years.
Professor Stokes-Lampard said the situation for GPs is not all negative, but more must be done to address the fall in GP numbers.
She added: “We are optimistic about the future of general practice: the financial commitment to primary and community care in the NHS long-term plan in England; the new five-year GP contract which promises that money will get to the front line; and pledges to ensure greater investment in technology are all part of a jigsaw that should help keep the NHS sustainable for the future. But GP numbers, which as this research shows are still falling, cannot be ignored.
“We need see more measures implemented to genuinely tackle soaring workload as a matter of urgency and efforts redoubled to cut red tape that diverts time away from patients, and we need to make the working environment in general practice supportive and sustainable, so that family doctors aren’t forced out of the profession. This would not just be in the best interests of GPs, but the NHS as a whole, and most importantly, our patients.”
MDS CEO Rohan Simon said: “MDS was created by GPs so we understand the pressure felt by our members – and what’s needed to look after their needs. We’re keen to ensure our GPs are happy and would welcome contact from anyone who needs further advice about coping with their workload.”
